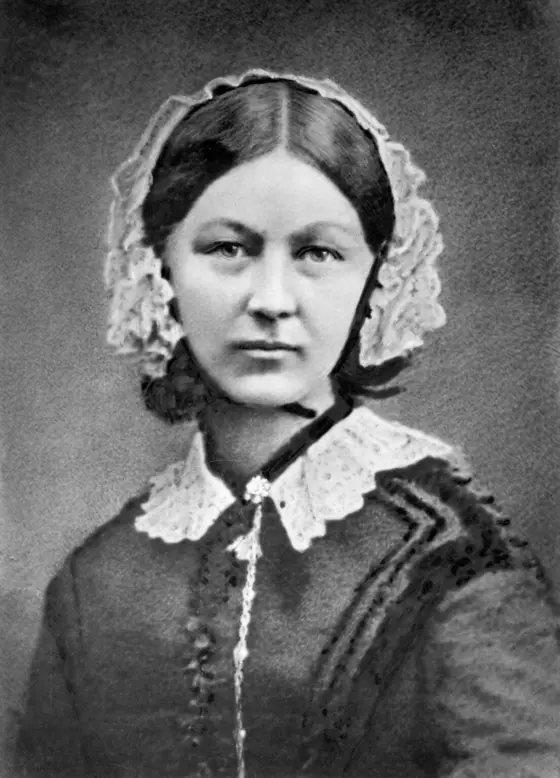The Woman the Victorian Era Did Not Expect
Florence Nightingale was born to wealth on 12 May 1820. Her father gave her an education unusual for any child of the era: Greek, Latin, history, mathematics, philosophy. That education was specifically unusual for a daughter. Victorian convention expected her to use it decoratively, then set it aside.
In February 1837, at age sixteen, she recorded a spiritual experience she described as a calling from God. She did not know yet to what purpose. She spent the following years in the social rounds expected of a woman of her class while privately reading hospital reports and public health statistics. In 1845, when she first asked to train as a nurse, her family refused.
Her most persistent suitor was Richard Monckton Milnes, a politician and poet who pursued her for nine years. She rejected his marriage proposal in 1849. Her diary records her reasoning: "My moral, active nature requires satisfaction, and that would not find it in this life."
The rejection was not romantic reluctance. It was a professional calculation. Marriage to Milnes would have ended any meaningful public work. She knew it and said so.
In July and October 1851, she traveled to Kaiserswerth, Germany, to train at the Institution of Protestant Deaconesses under Pastor Theodor Fliedner. Kaiserswerth was one of the few institutions in Europe offering systematic nursing instruction at the time. Nightingale was frank that its medical standards were limited, but the program gave her foundational clinical knowledge and, more importantly, a working model of what organized nursing care could look like. In 1853 she became superintendent of the Institution for the Care of Sick Gentlewomen in Distressed Circumstances in London, a private hospital she reorganized within months of arriving.
Scutari: What Nightingale Found at the Barrack Hospital
Florence Nightingale reduced the Barrack Hospital's mortality rate from 42-43% to 2.2% in six months by imposing sanitary reform, reorganizing supply chains, and restructuring military hospital wards. She arrived in November 1854 after Sidney Herbert, the Secretary of War and a close ally, asked her to lead a team of nurses to Scutari, a district of Constantinople (modern Istanbul).
The Barrack Hospital at Scutari was a catastrophe by any measure. The wards were overcrowded. Sewers ran open beneath the floors. Basic supplies were inadequate or absent. The hospital, in its degraded condition, was generating and distributing infectious disease more efficiently than any battlefield.
Nightingale imposed rigorous standards of cleanliness. She reorganized supply chains to get adequate food and materials to patients. She restructured the wards. Soldiers began recovering. The press noticed her lamp-lit night rounds and gave her the nickname that has endured: the Lady with the Lamp. The image was accurate as far as it went.
What the image missed was the administrative machinery behind it. Nightingale was not comforting men into health. She was redesigning the system that had been killing them.
The mortality rate, which had peaked at 42-43% of cases treated in February 1855, fell to approximately 2.2% within six months. Nightingale did not attribute the full reduction to her own interventions. She had pushed for a Sanitary Commission to address the hospital's structural problems and acknowledged that commission's contribution to the outcome. What her data confirmed was a fact her contemporaries found almost impossible to accept: 16,000 of the 18,000 British Crimean War deaths had come from preventable disease, not battle wounds.
The Numbers That Changed the Argument
Florence Nightingale invented the polar area diagram, also called the Nightingale Rose or coxcomb chart, to translate Crimean War mortality data into a form Parliament could not ignore. Working with the physician and statistician William Farr, she developed this new form of chart to communicate what her data showed.
The polar area diagram divided a circle into 12 equal-angle sections, one per month of the year. The area of each wedge grew or shrank in proportion to the death rate that month. She color-coded the causes: blue for preventable disease, red for battle wounds, black for other causes. The blue sections were enormous. The red sections, representing actual combat deaths, were small by comparison.
She sent the diagrams to Members of Parliament, government ministers, and Queen Victoria. A politician who would never read a mortality table could look at the polar area diagram and see, without calculation, that most of those men had died unnecessarily. The technique worked because it made the abstract undeniable. Nightingale is now recognized as a pioneer of data visualization, a field that would not formally exist for another century.
In 1858, the Royal Statistical Society elected her as its first woman Fellow, recognizing Florence Nightingale's statistical methods as a genuine contribution to public health epidemiology.
The Nightingale Training School: Where Modern Nursing Began
The Nightingale Home and Training School for Nurses, established at St Thomas' Hospital in London on 9 July 1860, was the first secular nursing school in the world. After the Crimean War, the British public raised £45,000 through public subscription for the Nightingale Fund. She used it for one purpose: to build the nursing school she had long envisioned.
What set the Nightingale Training School apart from anything that had existed before was its secular, credentialed structure. Religious orders, including Roman Catholic and Anglican deaconesses, had operated nursing programs before 1860. Those programs tied nursing to religious vocation, trained students in weeks or a few months, and produced nurses whose primary professional identity was that of a deaconess or sister, not a practitioner with transferable qualifications.
Nightingale's school enrolled students for a full year. The curriculum covered anatomy, physiology, chemistry, surgical nursing, sanitation, nutrition, ethics, and professional conduct. Students received lectures from hospital physicians, hands-on clinical training in the wards, and formal evaluation. They graduated with credentials that followed them professionally.
Between 1860 and 1903, the school certified 1,907 nurses. More significantly, Nightingale Training School graduates went on to establish nursing schools in Australia, Canada, the United States, and across Europe. The model traveled because it worked: the professionally trained nurse as a skilled practitioner, not a domestic servant or religious volunteer, became the global standard for nursing education.
Nightingale's transformation of nursing into a credentialed profession happened in parallel with the slow opening of medicine to women. The first woman to earn a medical degree faced a different but related set of institutional barriers, and the two stories together map the broader shape of women's entry into professional healthcare during the nineteenth century.
The Reformer Nobody Saw: Three Decades of Policy Work from a Sickbed
Florence Nightingale returned from the Crimea in August 1856 at age 36, traveling under an assumed name to avoid public ceremony. Within a year she had collapsed. The modern diagnosis is brucellosis with associated spondylitis, a bacterial infection contracted in the Crimea that produces chronic fatigue, joint pain, and intermittent fever. She also experienced severe depression throughout much of this period.
From her rooms at 10 South Street, Mayfair, she produced detailed sanitary reform reports for British India, running to hundreds of pages, based on data sent to her from a subcontinent she never visited. She advocated for army medical reform. She influenced hospital design across Britain, Canada, Australia, and beyond.
In 1859, Nightingale published Notes on Nursing: What It Is and What It Is Not, the first nursing textbook written for educated women and household caregivers rather than for professionals alone. The same year she published Notes on Hospitals, which advanced the case for the pavilion design: separate ward blocks with high ceilings, cross-ventilation, and large windows. She argued, correctly, that this architectural approach would reduce infection rates through improved airflow. Her hospital design principles shaped construction decisions across Britain and internationally.
Her lifetime written output reached over 130,000 letters.
The brucellosis began lifting in the early 1880s. Her final decade brought declining health, eventual blindness, and slowing output. In 1907, Nightingale received the Order of Merit, one of Britain's highest civilian honors, becoming the first woman to hold it. She died on 13 August 1910, at her Mayfair home. She was 90. She had declined burial in Westminster Abbey; she is buried in the churchyard of St Margaret's Church, East Wellow, Hampshire.
What Florence Nightingale's Firsts Actually Mean
Florence Nightingale was elected Fellow of the Royal Statistical Society in 1858, the first woman to hold that distinction. She received the Order of Merit in 1907, again the first woman recipient. She founded the first secular nursing school in the world in 1860 at St Thomas' Hospital, London. International Nurses Day is observed annually on 12 May, her birthday; the International Council of Nurses formally established the observance in January 1974.
The Florence Nightingale Medal, awarded by the International Committee of the Red Cross, remains the highest international distinction a nurse can receive. The Nightingale Pledge serves as nursing's professional oath. The Florence Nightingale Faculty of Nursing and Midwifery at King's College London, the direct institutional successor to her original training school, continues to prepare nurses today.
Scholar Lynn McDonald, editor of the Collected Works of Florence Nightingale at the University of Guelph, has documented the full range of her statistical and policy contributions, establishing Nightingale as a foundational figure in public health epidemiology alongside her role in nursing education.
What ties these together is a single consistent act: Florence Nightingale built structures. The polar area diagram, the Nightingale Training School, the nursing textbooks, the sanitary reform reports, the 130,000 letters. The lamp was real, but it was never her instrument.
Frequently Asked Questions
Why is Florence Nightingale called the founder of modern nursing?
Nightingale created the first secular, structured nursing education program, turning nursing from an informal trade into a professional discipline with a curriculum, credentials, and an institutional home. Before her Nightingale Training School opened in 1860, nursing had no formal education pathway and was widely seen as unsuitable for educated women. Her textbook, her school's global reach, and her statistical advocacy for sanitary reform set the professional and intellectual foundations that modern nursing still builds on.
Why is Florence Nightingale called the "Lady with the Lamp"?
The nickname came from her practice during the Crimean War of walking the wards of the Barrack Hospital at Scutari at night, carrying a lamp to check on patients. British soldiers and the press adopted the image, and it became the most enduring symbol of her wartime work. The nickname was accurate but incomplete: her real instruments were sanitary reform, mortality data, and institutional design.
What is Florence Nightingale's most important invention?
Her most significant intellectual contribution is the polar area diagram, also called the Nightingale Rose or coxcomb chart. She developed it after the Crimean War to communicate mortality data to Parliament and the public in a form that was impossible to ignore. By coding causes of death in color and sizing sections proportionally to death rate, she made it visually undeniable that most soldier deaths had been preventable. The technique predates the modern field of data visualization by over a century.
How did Florence Nightingale change hospitals?
She changed hospitals on two levels: sanitation practice and architectural design. During the Crimean War she imposed cleanliness standards, improved ventilation, and reorganized nutrition and supply chains at Scutari, reducing the mortality rate from approximately 42-43% to 2.2% in six months. In her 1859 book Notes on Hospitals, she made the case for the pavilion design: separate ward blocks with high ceilings and cross-ventilation, which she argued correctly would reduce infection rates through airflow. Her influence shaped hospital construction across Britain and internationally.
When did Florence Nightingale die, and what honors did she receive?
Florence Nightingale died on 13 August 1910, in her Mayfair home in London, at the age of 90. In 1907 she became the first woman to receive the Order of Merit, one of Britain's highest civilian honors. She was elected a Fellow of the Royal Statistical Society in 1858, the first woman to hold that distinction. She had declined burial in Westminster Abbey; she is buried in the churchyard of St Margaret's Church, East Wellow, Hampshire.